 |
 |
- Search
| Intest Res > Volume 17(4); 2019 > Article |
|
Abstract
Background/Aims
Methods
Results
NOTES
FINANCIAL SUPPORT
The authors received no financial support for the research, authorship, and/or publication of this article.
AUTHOR CONTRIBUTION
Conceptualization: Behm BW. Data curation: Wang J, Nakamura TI. Formal analysis: Wang J. Methodology: Behm BW, Wang J. Project administration: Behm BW, Tuskey AG. Visualization: all authors. Writing - original draft: Wang J. Writing - review & editing: Wang J, Nakamura TI, Tuskey AG, Behm BW. Approval of final manuscript: all authors.
Fig. 1.
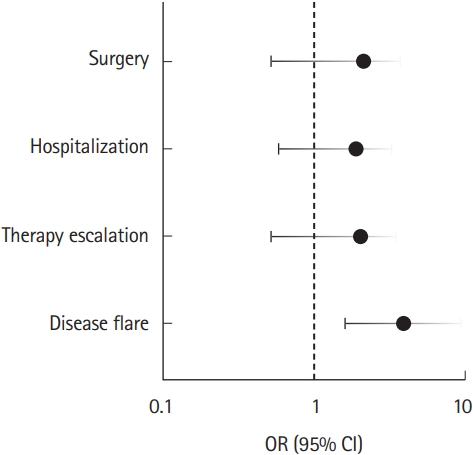
Table 1.
| Characteristics | Major polypharmacy (n = 136) | Minor polypharmacy (n = 187) | No polypharmacy (n = 134) | P-value |
|---|---|---|---|---|
| Age (yr) | 59.29 ± 1.33 | 49.72 ± 1.13 | 48.24 ± 1.34 | < 0.001 |
| Sex | 0.019 | |||
| Female | 79 (58) | 95 (51) | 55 (41) | |
| Male | 57 (42) | 92 (49) | 79 (59) | |
| Average number of drugs | 7.40 ± 0.15 | 2.86 ± 0.13 | 0.52 ± 0.15 | < 0.001 |
| Montreal classification | 0.750 | |||
| E1 (proctitis) | 11 (8) | 19 (10) | 16 (12) | |
| E2 (left-sided) | 52 (38) | 65 (35) | 50 (37) | |
| E3 (extensive) | 73 (54) | 103 (55) | 68 (51) | |
| Disease duration (yr) | 8.63 ± 0.69 | 6.98 ± 0.60 | 6.31 ± 0.70 | 0.051 |
| Tobacco use | 12 (9) | 20 (11) | 8 (6) | 0.330 |
| Alcohol use | 51 (38) | 77 (41) | 58 (43) | 0.610 |
| Functional GI disordersb | 24 (18) | 5 (3) | 6 (4) | < 0.001 |
| Psychiatric illnessc | 43 (32) | 29 (16) | 17 (13) | < 0.001 |
a Differences across polypharmacy classes were assessed using chi-square test for categorical variables and ANOVA for continuous variables. Major polypharmacy, >5 non-UC medications; minor polypharmacy, 2-4 non-UC medications; no polypharmacy, <2 non-UC medications. At 5-year follow-up; major polypharmacy (n=57), minor polypharmacy (n=113), no polypharmacy (n=95).
Table 2.
| Medication | Disease flare | Therapy escalation | Hospitalization | Surgery |
|---|---|---|---|---|
| Opioids | 2.18 (0.25-18.73) | 0.75 (0.21-2.76) | 3.84 (1.09-13.57) | 3.04 (0.89-10.39) |
| Antidepressants | 1.65 (0.57-4.81) | 0.68 (0.26-1.76) | 1.85 (0.76-4.51) | 1.88 (0.72-4.26) |
| NSAIDs | 1.08 (0.35-3.28) | 1.71 (0.68-4.30) | 0.45 (0.16-1.31) | 0.24 (0.05-1.08) |
| Benzodiazepines | 0.97 (0.29-3.28) | 0.69 (0.24-2.00) | 1.34 (0.49-3.66) | 1.36 (0.46-4.01) |
| Prebiotics | 0.48 (0.08-2.77) | 8.40 (1.44-49.03) | 0.46 (0.05-4.07) | NAb |
| Probiotics | 2.01 (0.53-7.65) | 1.08 (0.39-3.01) | 0.61 (0.22-1.71) | 0.83 (0.28-2.43) |
Table 3.
| Drug-drug interaction | Incidence, No. (%) | Adverse effect |
|---|---|---|
| Mesalamineb & PPI | 51 (12.5) | Class D-PPIs may diminish the therapeutic effect of 5-ASA medications via alteration in GI pH |
| Mesalamine & calcium carbonate | 40 (9.8) | Class D-antacids may diminish the therapeutic effect of 5-ASA medications via alteration in GI pH |
| Benzodiazepines & opioids | 38 (9.3) | Class D-CNS depressants may enhance the CNS depressant effect of opioids |
| Musculoskeletal relaxantc & opioid | 37 (9.1) | Class D-CNS depressants may enhance the CNS depressant effect of opioids |
| Calcium carbonate & systemic steroids | 19 (4.7) | Class D-antacids may decrease the bioavailability of oral corticosteroids |
a Class D or X interactions—defined as “consider therapy modification” and “avoid combination,” respectively—according to Lexicomp®. Drugs interactions (Lexicomp®; Wolters Kluwer Health, Inc. Hudson, OH, USA, available at http://online.lexi.com).
REFERENCES
- TOOLS








